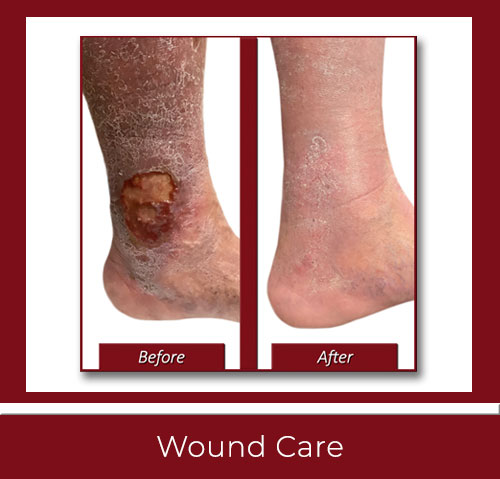
Wound Care Center With the Best Vascular Specialists Serving Milford, New Haven, Bridgeport, Stamford and All Of Southern Connecticut
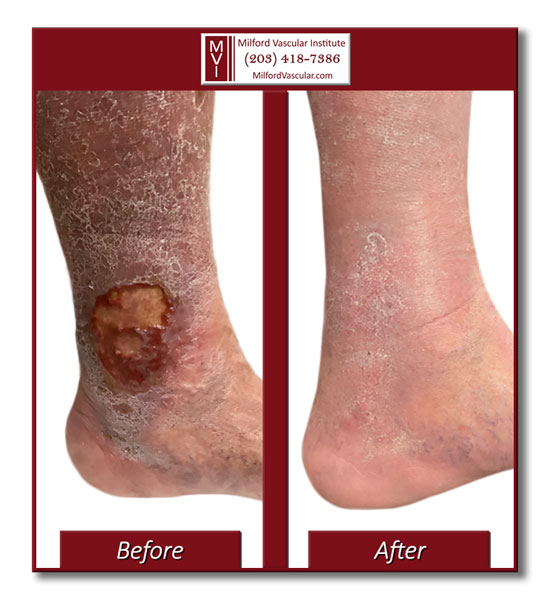
Wound care center at Milford Vascular Institute provides state-of-the-art treatments for non-healing wounds and ulcers caused by venous disease and arterial disorders.
We use the most advanced treatments to help restore healthy circulation to the wound, while at the same time applying the appropriate dressings, medications, and skin grafts to encourage quick healing.
Negative pressure applications such as wound VAC treatments and PICO wound management devices are also used to help minimize the risk of infection and accelerate the healing process.
WHY PROPER WOUND CARE IS CRUCIAL FOR YOUR HEALTH
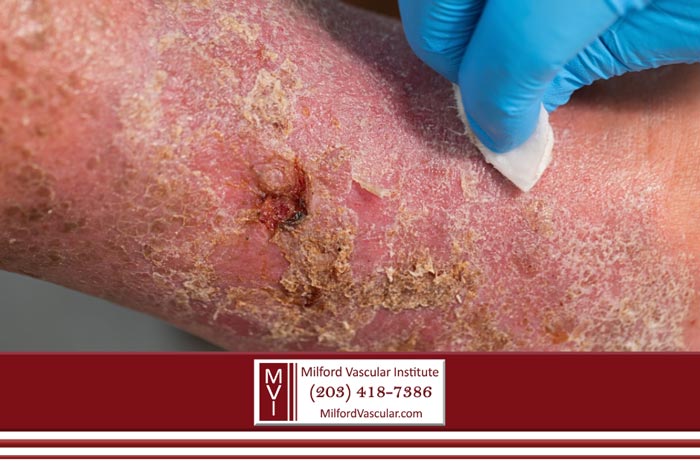
Poor circulation through the arms and legs can eventually result in skin ulcers that don’t heal.
Non-healing skin ulcers can result in long-term health problems including extreme pain, loss of function and mobility, and prolonged hospitalization.
Left untreated, irreparable skin damage and infections can occur, that can eventually lead to amputation.
That is why it is crucial to get proper wound care at a wound care center, as well as determine the root cause of the problem, and receive proper treatment.
Wound Care Patient Testimonial
Patient Tom Shares His Story About Having Venous Insufficiency Treatment and Wound Care at Milford Vascular Institute
What Causes Non-Healing Wounds?
LEFT UNTREATED, VENOUS INSUFFICIENCY CAN CAUSE SKIN ULCERS THAT DO NOT HEAL
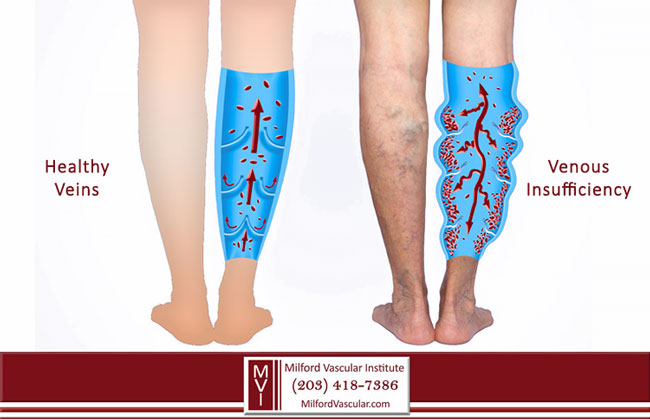
Damaged vein valves in the legs can cause blood to pool in the lower legs, a condition known as venous insufficiency.
Venous insufficiency interferes with healthy blood flow from the lower extremities towards the heart, resulting in poor circulation through the legs.
The lack of healthy circulation in the legs can eventually cause the skin on the legs to die, resulting in the formation of venous ulcers. Without healthy blood circulation, venous ulcers can continue to worsen rather than heal.
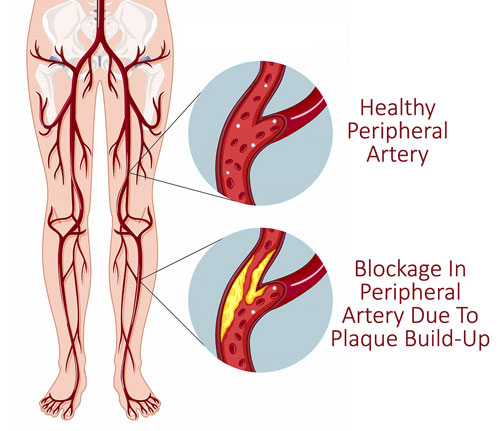
LEFT UNTREATED, PERIPHERAL ARTERIAL DISEASE CAN CAUSE NON-HEALING SKIN ULCERS
Clogged arteries in the arms and legs can prevent nutrients and oxygen to be delivered to the extremities, a condition known as peripheral arterial disease.
Blocked leg arteries interfere with healthy blood supply flowing from the heart to the lower legs, resulting in poor circulation in the legs, feet and toes.
The lack of healthy blood supply to the lower extremities can eventually cause the skin on the lower legs and feet to die, resulting in the formation of arterial ulcers, also called ischemic ulcers. Without healthy blood circulation, arterial ulcers can continue to worsen rather than heal, and can eventually require amputation.
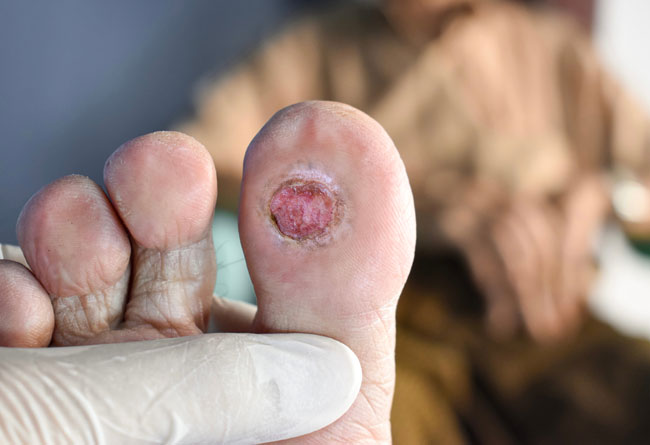
DIABETES MAKES PEOPLE MORE SUSCEPTIBLE TO DEVELOPING NON-HEALING WOUNDS
Research suggests that 15% of people who have diabetes will experience diabetic foot ulcers in their lifetime.
Diabetes interferes with wound-healing and can quickly cause wounds or ulcers to become infected.
Diabetic foot ulcers typically develop on the bottom of the foot and on the toes.
Gangrene can set in quickly, resulting in the need for amputation.
State-of-the-Art Wound Care
Here at Milford Vascular Institute, our top-rated vascular specialists who are experts in wound care serve Milford, New Haven, Bridgeport, Stamford and all of Southern Connecticut, using the most advanced wound treatments, as provided in a wound care center. We provide close monitoring and treatment for cellulitis and wound infections, as well as antibiotic therapy when needed.
MVI WOUND CARE METHODS
Here at MVI, we also do evaluation of circulation for local podiatrists when patients have diabetic foot ulcers to make sure they have adequate blood flow to ensure wound healing. This would include ABI and arterial ultrasound.
We can also refer you to the wound center when needed, or arrange for visiting nurses for home wound care.
Why Choose

When you choose Milford Vascular Institute for your non-healing wound care, you can rest assured that you are getting the very best possible care available in all of New Haven County. Our vascular specialists are highly skilled in providing the most advanced, comprehensive wound care available anywhere.
At MVI, wound care is provided under the direction of board certified vascular surgeon Dr. David Esposito and Dr. Paul Davis, who is board certified in diagnostic radiology, and vascular and interventional radiology.
Dr. Esposito and Dr. Davis are top-rated experts in vascular treatments. They are always at the forefront of technology in the vascular health field to ensure they are providing the best, cutting-edge wound care and treatments to their community.
Board certified Physician Assistant, Karin Augur board certified Adult Nurse Practitioner, Thomas Rank and board certified Family Nurse Practitioner, Brittany Reilly specialize in understanding and treating the root cause of your non-healing wounds, whether it be due to venous disease, or arterial blockages.
Restoring healthy circulation is the first step to helping to heal your non-healing wounds, venous ulcers, arterial ulcers or diabetic foot ulcers. Using a combination of state-of-the-art wound care treatments, you can put your trust in our vascular specialists to heal your non-healing wounds.

With over 70 years of combined experience in diagnosing, preventing and treating vascular diseases, our outstanding group of highly trained and skilled providers have dedicated their lives to caring for you.
With over 20 years in practice, at Milford Vascular Institute, our staff is committed to excellent patient care, always treating our patients with respect and compassion because WE CARE.

Our MVI Team ~ Always Treating You Like Family
If you’ve started to develop a venous ulcer, an arterial ulcer, or noticed that your wound is simply not healing on its own, it is important to have an evaluation with a vascular specialist as soon as possible. If left untreated, skin ulcers and wounds that do not heal can result in permanent tissue loss, gangrene, and even amputation.
Through a simple in-office consultation, we can determine the root cause of your ulcers and non-healing wounds, and put a treatment plan in place to restore healthy circulation and heal your skin wounds.
To schedule a consultation with one of our top-rated vascular specialists here at Milford Vascular Institute, give us a call today at (203) 418-7386. It will be our pleasure to care for you.

