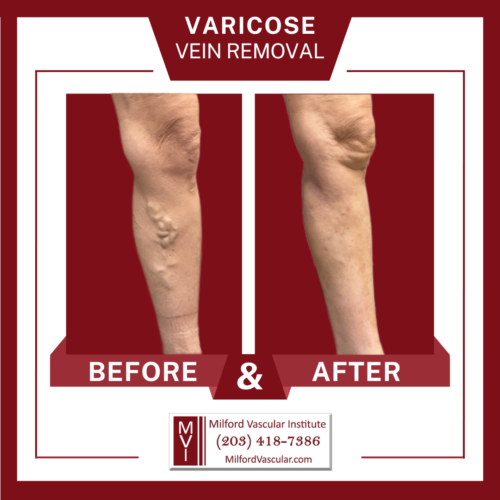
Varicose Veins Indicate A Serious Medical
Condition That Can Lead To Deadly Blood Clots If Left Untreated

Varicose veins on the legs indicate a deeper vascular disease known as venous insufficiency. Over 24 million Americans are suffering from varicose veins.
Left untreated, varicose veins and venous insufficiency can cause debilitating symptoms such as leg swelling, leg heaviness and leg cramps.
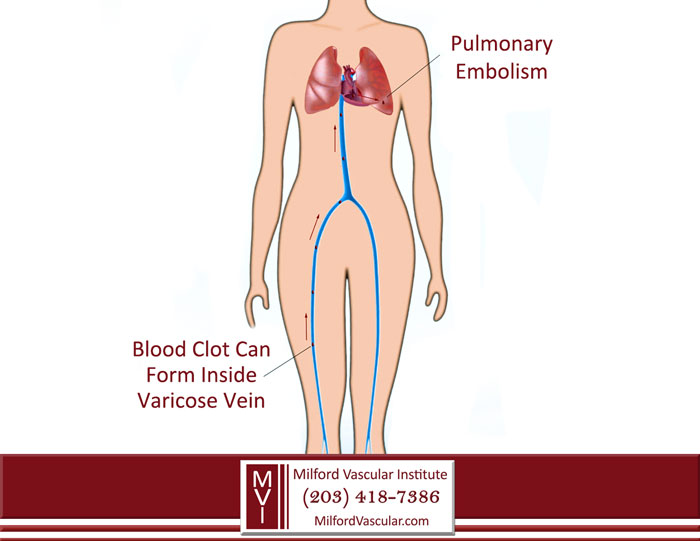
Blood clots can form inside diseased veins, travel to the lungs and cause a potentially deadly pulmonary embolism.
So, it is important to have your varicose veins checked by a vascular specialist as soon as possible.
LEFT UNTREATED VARICOSE
VEINS CAN LEAD TO A DEADLY PULMONARY EMBOLISM
So, if you have developed varicose veins on your legs, it is recommended to have a vein consultation to help determine if your enlarged veins are due to venous insufficiency.
If you do have venous insufficiency, treatment is very important to prevent your condition from worsening, and to prevent potentially deadly blood clots from forming.
What Are Varicose Veins?
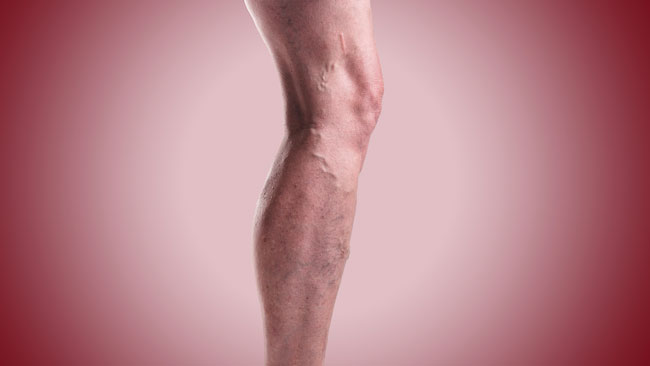
Varicose veins are the enlarged, twisted veins you can see protruding, usually on the legs. They can also exist deep in the legs where they are not visible.
These bulging veins most commonly occur in the legs due to gravity. Gravity is constantly pulling the blood downwards, into the leg veins.
This added pressure in the leg veins can cause veins to expand and become varicose.
Board Certified Vascular Surgeon Dr. Esposito Explains Varicose Veins
“A lot of people look at varicose veins, and they think that they’re a cosmetic problem, and sometimes they are.
But most of the time, varicose veins are a sign of something more serious that’s going on underneath the surface. And that something going on underneath the surface is what we call venous insufficiency.
Varicose veins can cause pain, swelling, itching, tenderness. Can lead to phlebitis or thrombophlebitis and blood clots. So my recommendation is that if you have varicose veins, it’s very important to have them checked by a vascular specialist.”
~ Dr. David Esposito
Board Certified Vascular Surgeon
“If you come to Milford Vascular Institute with varicose veins, the first thing we’ll do is perform a dedicated vascular ultrasound exam to determine if you have venous insufficiency.
If you do have venous insufficiency, we have various techniques where we can use lasers or microwave energy. We can do injections, we can remove veins, and it’s all done in the office.
It’s all done under local anesthesia with almost no recovery, minimal time down, very little risk, very little discomfort.”
~ Dr. David Esposito
Board Certified Vascular Surgeon
What Causes Varicose Veins In Legs?
The veins’ job is to take blood from our feet to our heart. The problem is gravity is pulling all of the blood constantly to our feet.
The veins have tiny valves in them that help counter this effect of gravity. As the blood moves toward the heart, the valves close, and the blood won’t go backwards. It keeps going in the right direction.
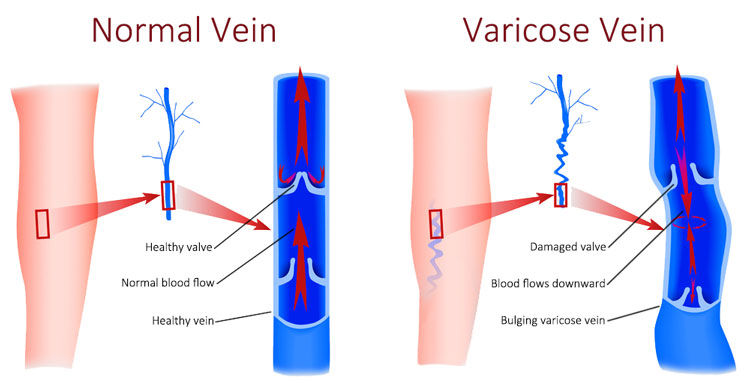
For some people, however, these valves wear down and become damaged. The valves leak, allowing blood to flow downwards and pool in the lower legs. This leads to a buildup of pressure in the veins.
The superficial veins then start to become engorged from that high pressure. And varicose veins start to become visible on the skin.
Some people are more prone to developing varicose veins for various reasons, such as:
Why Are Women More Prone To Having Varicose Veins?
In general, women are at a higher risk of developing varicose veins on their legs than men.
Hormonal changes that occur during pregnancy, as well as the higher amount of blood in the body puts strain on the vein walls, increasing the chance of developing varicose veins.
In addition, if a woman has been pregnant multiple times, her risk of developing varicose veins also increases.
PREGNANCIES INCREASE THE CHANCE OF DEVELOPING VARICOSE VEINS

What Are The Symptoms Of Varicose Veins?
Varicose veins on the legs can cause a multitude of various symptoms, which only get worse with time if untreated. They include:
If you are experiencing any of these symptoms associated with varicose veins, it is recommended to have a vein consultation with a vascular specialist as soon as possible.
Providing The Most Advanced Varicose Vein Treatments Available Anywhere
Here at Milford Vascular Institute, our top-rated vascular specialists serving New Haven, Bridgeport, Stamford and all of Southern Connecticut, use the most advanced minimally-invasive vein treatment techniques available anywhere in the world to treat your varicose veins and the underlying venous insufficiency.
BOARD CERTIFIED VASCULAR AND INTERVENTIONAL RADIOLOGIST DR. DAVIS PERFORMING VARICOSE VEINS SURGERY
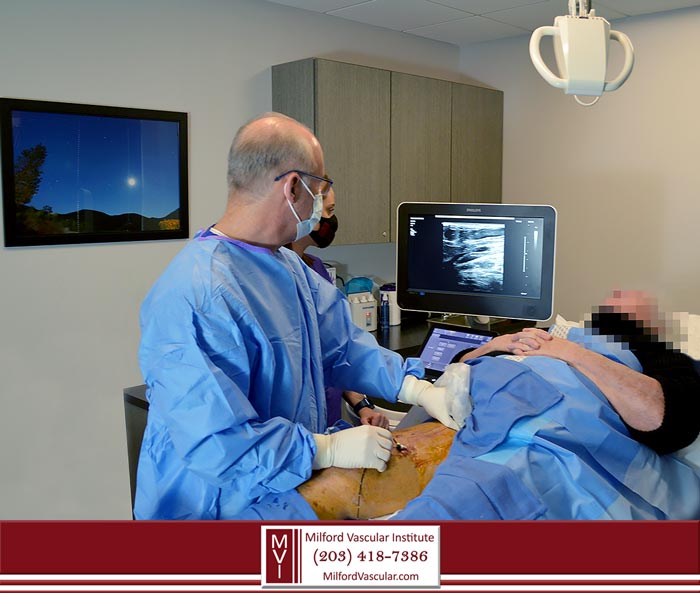
The deeper veins that are causing venous insufficiency must first be treated, since they are the reason your varicose veins have developed. Our vascular specialists perform low-risk procedures right in our office. They are performed under local anesthesia, and they include:
- radiofrequency ablation
- Varithena® microfoam injection
- VenaSeal™ vein closure procedure
- laser vein ablation
After the deeper malfunctioning veins have been closed using the above procedures, the underlying problem has been treated. However, some large varicose veins may remain and will need to be physically removed using the ambulatory phlebectomy procedure.
Varicose veins surgery is performed through a small puncture in the leg so it does not require any sutures or staples, and only the diseased veins are closed. Healthy blood flow is restored through your other well-functioning veins.
These procedures allow for quick recovery time and leave minimal to no scarring in the treatment area.
Varicose Veins Surgery Patient Testimonials
Patients Share Their Stories About Having Varicose Vein Removal at Milford Vascular Institute
Why Choose

When you choose Milford Vascular Institute for vein treatment you can rest assured that you are getting the very best possible vascular care available in all of New Haven County. Our vein specialists are highly skilled in providing the most advanced, minimally-invasive vein treatments available anywhere.
At MVI, vein treatments are provided under the direction of board certified vascular surgeon Dr. David Esposito and Dr. Paul Davis, who is board certified in diagnostic radiology, and vascular and interventional radiology.
Dr. Esposito and Dr. Davis are top-rated experts in vein treatments. They are always at the forefront of technology in the vascular surgery field to ensure they are providing the best, cutting-edge vein treatments to their community.
Board certified Physician Assistant, Karin Augur, board certified Adult Nurse Practitioner, Thomas Rank and board certified Family Nurse Practitioner, Brittany Reilly specialize in varicose vein removal, helping to restore healthy blood flow through your legs so they can look and feel their best.

With over 70 years of combined experience in diagnosing, preventing and treating vascular diseases, our outstanding group of highly trained and skilled providers have dedicated their lives to caring for you.
With over 20 years in practice, at Milford Vascular Institute, our staff is committed to excellent patient care, always treating our patients with respect and compassion because WE CARE.

Our MVI Team ~ Always Treating You Like Family
If you’ve started to notice varicose veins developing on your legs, it is important to have an evaluation with a vascular specialist, because varicose veins are an indication of a deeper vascular problem called venous insufficiency.
Through a simple in-office ultrasound, we can determine if your varicose veins are due to venous insufficiency. If they are, we can treat you accordingly, using the most advanced vein treatment methods available anywhere.
Treatments are performed right in our offices using minimally-invasive techniques so you can enjoy no downtime and quick recovery.
To schedule a vein consultation with one of our top-rated vascular specialists here at Milford Vascular Institute, give us a call today at (203) 418-7386. It will be our pleasure to care for you.